| Lung cancer Classification | |
| Small cell Lung cancer | Non Small cell Lung cancer (NSCLC) |
|
|
Investigation:
Aims of investigation are
-
- to confirm the diagnosis,
- to establish the histological cell type
- to define the extent of the disease.
- to see paraneoplastic manifestation
- to see comorbidities
| Investigation | Finding |
| CBC, PBF |
|
| Sputum microscopy for malignant cell |
|
| Chest X Ray
|
|
| CT chest |
|
| Biopsy and histopathology | |
|
|
| Pleural fluid aspiration with pleural biopsy (thoracoscopy) | |
| FNAC or biopsy from LN, liver, skin nodule | |
| For staging | |
| Combined CT and whole-body FDG-PET |
|
|
|
| molecular testing: next-generation sequencing (NGS) for gene mutation |
|
| To assess baseline for aggressive treatment | |
|
ECG, Echocardiography Lung function test |
|
| S creatinine, urea, electrolytes |
|
| S calcium, albumin, Phosphate, PTH |
|
| ALT, ALP, PT, bilirubin |
|
| TSH, blood sugar | |
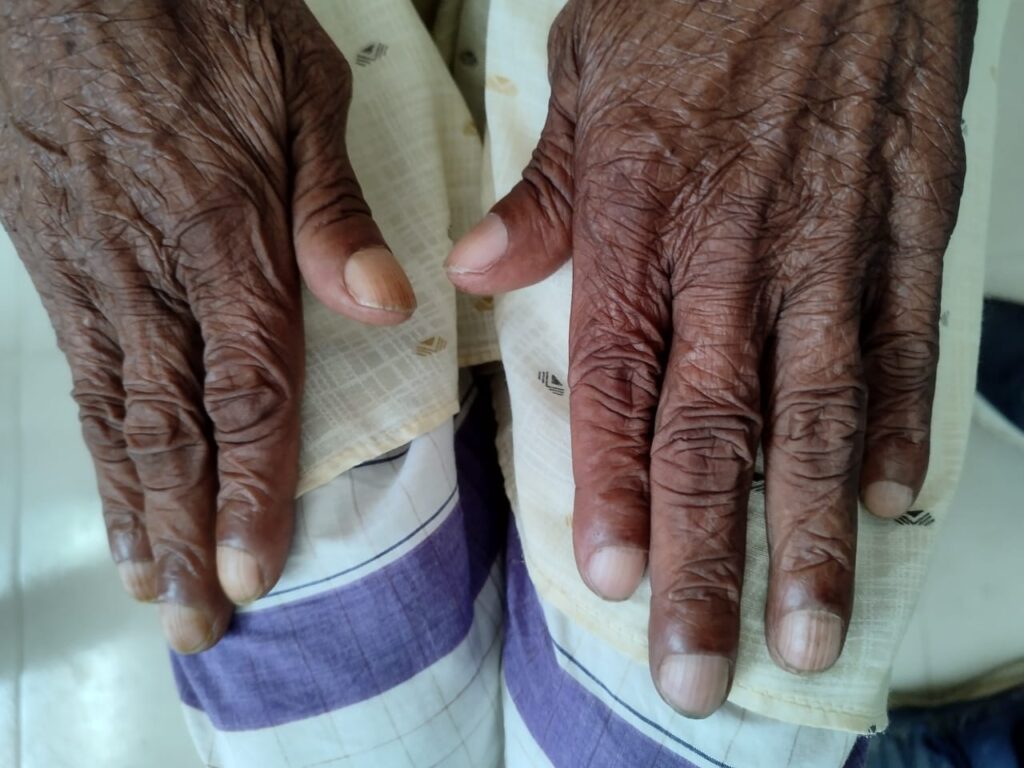
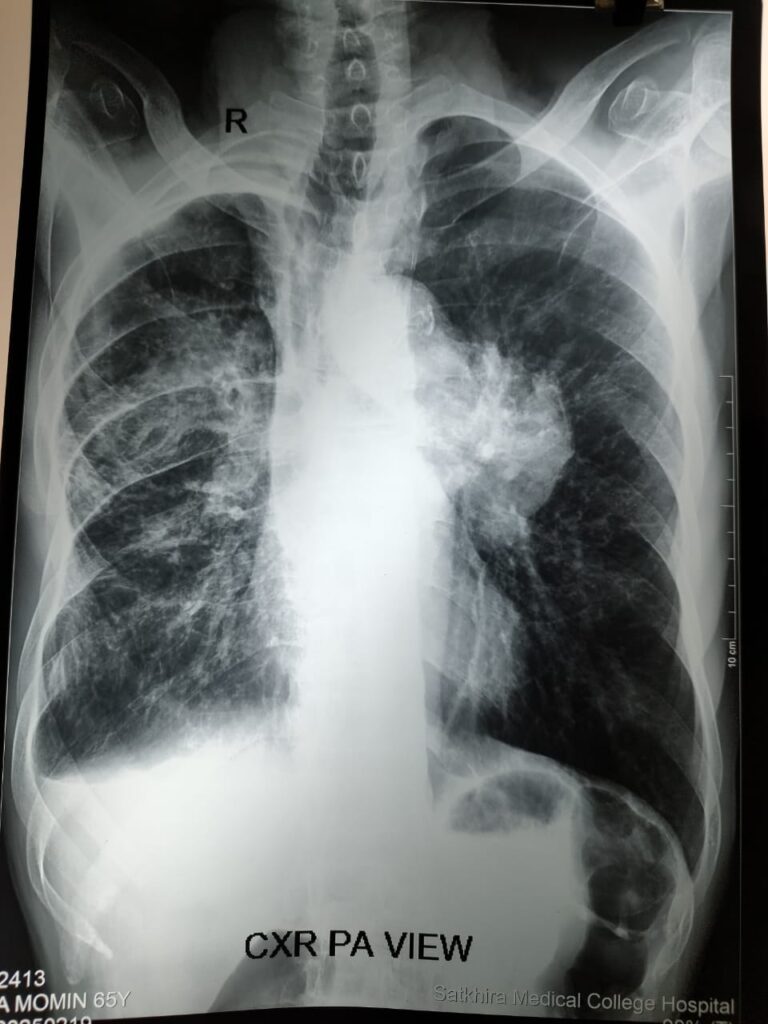
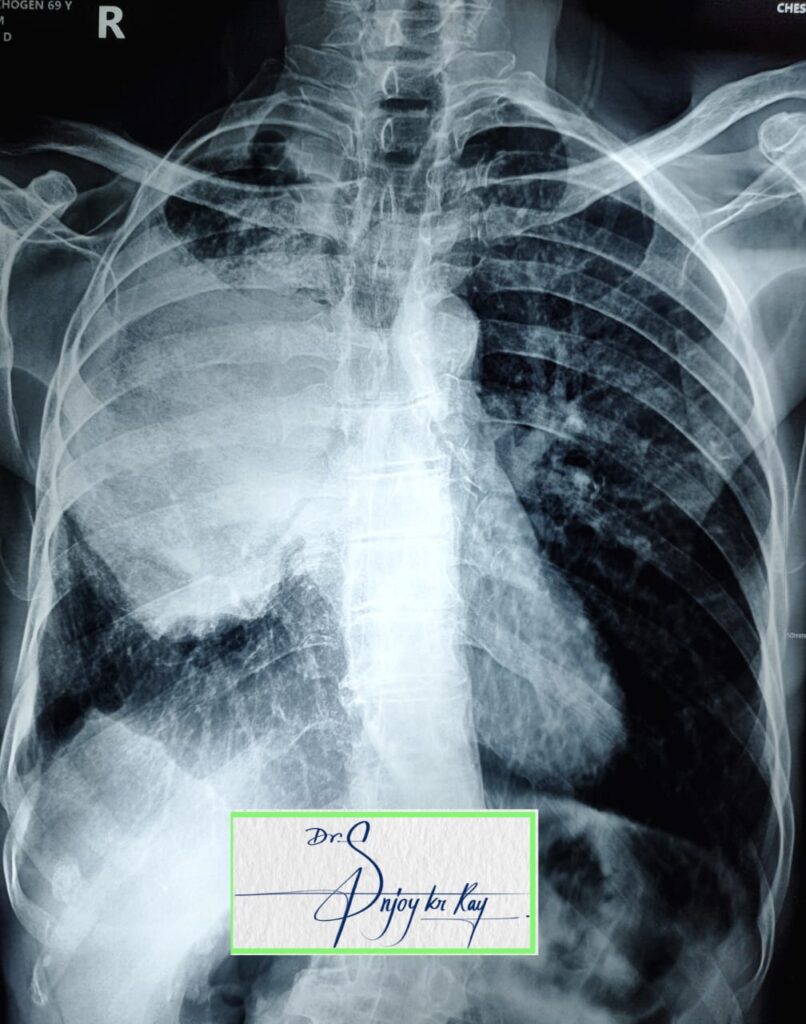
Staging in short:
| Stage | Definition |
| Stage I | N0 (no lymphadenopathy), tumor confined within visceral pleura (<4 cm) |
| Stage II | N1 [Ipsilateral hilar, tumor size < 5 cm (or > 5 cm with N0] |
| Stage III |
Ipsilateral mediastinal or subcarial, OR contralateral or supraclavicular Tumor size > 7 cm or invading heart, vessel, esophagus, caria etc |
| Stage IV | Lung metastasis/ Effusio / Extrathoracic metastasis |
Treatment:
| Stage of NSCLC | Treatment |
| I | Surgery |
| II | Surgery → adjuvant chemotherapy |
| III | Surgery → chemo with or without radiotherapy |
| IV
*EGFR: Epidermal Growth Factor Receptor |
Radiotherapy Systemic therapy (TIC): which may consist of
|
Surgical management: 5-year survival rates for
- Stage I disease: over 80%
- stage II disease: 70% in stage II disease,
Palliative treatment:
- Radiotherapy:
-
- SVCO, recurrent haemoptysis
- pain caused by chest wall invasion or by skeletal metastasis.
- obstruction of the trachea and main bronchi
- For major airway obstruction
-
- bronchoscopic laser treatment to clear tumor tissue.
- Endobronchial stents to maintain airway patency in case of extrinsic compression by malignant nodes.
General aspects of management
- managed in specialist centers by multidisciplinary teams, including
-
- oncologists, thoracic surgeons, respiratory physicians and specialist nurses.
- Effective communication, pain relief and attention to diet are important.
- For depression and anxiety → specific therapy.
- Management of non-metastatic endocrine manifestations
- For malignant pleural effusion
- intercostal drain;
- long-term indwelling pleural catheters
- pleurodesis with sclerosing agents such as talc.
Prognosis
- The overall prognosis is very poor
- mortality rate from diagnosis
- 1 year mortality rate approximately 60%
- 5 year mortality rate over 80%
- The best prognosis is for
- well-differentiated squamous cell carcinoma that have not metastasised and are amenable to surgical resection.
*** *** ****
SCLC: Chemo + Radiotherapy
- SCLC is a highly aggressive disease characterized by its rapid doubling time, high growth fraction, early development of disseminated disease, and dramatic response to first-line chemotherapy and radiation.
- In general, surgical resection is not routinely recommended for patients because even patients with LD-SCLC still have occult micrometastases.
Chemotherapy agents (davidson): VCDE
- vincristine (oncovin brand name!!)
- cyclophosphamide, cisplatin
- doxorubicin
- etoposide
Prognosis (SCLC): median survival from 3 months to over a year.
Eye features of lung cancer:
- Horner syndrome
- Cancer associated retinopathy
